Infosheet: Blastomycosis for Dog Owners

To download a PDF of this document, please click here: https://www.oahn.ca/wp-content/uploads/2022/02/Blasto-Infosheet-Format-vF.pdf
What is blastomycosis?
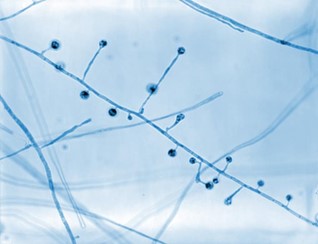
Blastomycosis is an infection caused by a fungus called Blastomyces dermatitidis. It most commonly infects the lungs, but the fungus can spread from there to many other organs in the body as well. The fungus can also rarely infect open wounds.
Blastomyces dermatitidis is typically found in warm, moist soil along riverbeds in certain regions of North America, particularly in the east in areas bordering the Great Lakes and the Ohio River and Mississippi River. In Ontario, the highest risk regions are around Georgian Bay, northwestern Ontario and the Ottawa region.

How is blastomycosis spread?
Blastomycosis can affect people as well as animals, but it is not easily spread between people and animals, because the infectious mold form of the fungus is found in the soil. When contaminated soil is disturbed, fungal spores can be released into the air and are then inhaled into the lungs. When it infects a person or animal, the fungus takes on a different form (yeast) which is not easily spread between individuals, although bites that break the skin can be a risk. Basic precautions (e.g. gloves, hand hygiene) should be used if contact with an infected, draining wound is needed.
Dogs tend to be more susceptible to infection than humans. Cats can also be infected but this is much less common.
What are signs of blastomycosis in dogs?
Not every dog (or person) who is exposed to the fungus gets sick. When signs do occur, they often take a few weeks to a few months to appear. The initial signs are often the same as other lung infections, including:
- Fever, depression, loss of appetite
- Cough, increased respiratory rate or effort
- Weight loss
Other signs may occur if the fungus spreads to other parts of the body, including blindness, lameness, seizures, inflamed testicles and enlarged lymph nodes. Draining skin lesions may also occur, especially if the fungus enters the body through broken skin.

How is blastomycosis in dogs diagnosed?
The fungus that causes blastomycosis is often readily detected by microscopic examination of fluid (e.g. from a wound or lymph node) or a tissue biopsy. Blood and urine can also be tested for fungal antigen, which can help support a diagnosis of blastomycosis.
Chest radiographs often show a characteristic pattern in the lungs consistent with fungal pneumonia, and are important for gauging how advanced the infection is at the time.
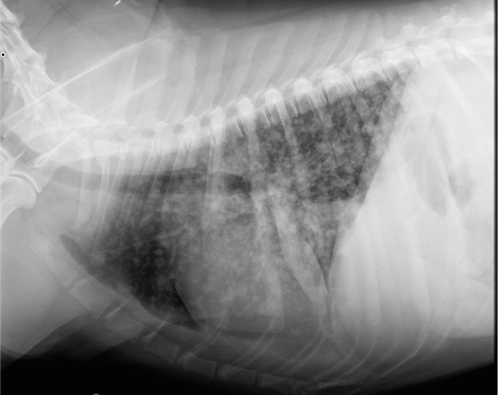
There is also a test (AGID) to detect antibodies to B. dermatitidis in the bloodstream, but this only indicates that the dog was exposed, not that it’s infected. Up to 30% of dogs with confirmed clinical infection may test negative for antibodies at the time of presentation.
How is blastomycosis in dogs treated?
The infection can be treated in many cases using antifungal medication, but typically requires 4-6 months of treatment. The key is to diagnose the disease as soon as possible and start treatment right away.
Approximately 50-75% of dogs with blastomycosis recover. Dogs with advanced disease or other conditions are less likely to survive. Relapse of the infection can occur in some cases, so regular follow-up exams and testing are also very important.
What can I do to protect my pets from blastomycosis?
There is no vaccine against blastomycosis. The best way to prevent infection is to prevent exposure to the moist soil and decaying material along riverbanks and other areas where the fungus is most often found. Environmental testing is not considered useful, and there is no way to eliminate the fungus from the soil. Keeping your pets healthy, vaccinating against other respiratory diseases and preventing parasitic infections can help your pet fight off infection if there is low-level exposure.
If your dog spends a lot of time outside, especially where it might sniff or dig in moist soil along riverbeds in areas where this fungus is known to occur, then your dog may be at higher risk for blastomycosis. If your dog gets sick, be sure to let your veterinarian know about this kind of exposure so that testing for blastomycosis can be done as soon as possible, before infection becomes advanced and harder to treat. If you travel to areas where blastomycosis is more common, it is important for your veterinarian to know that. Blastomycosis sometimes occurs in multiple dogs from the same environment at the same time, or from dogs in the same environment years later. If you know other dogs from your local area or an area you visit have had blastomycosis, this should also be conveyed to your veterinarian, so they are aware that there might be increased risk of Blastomyces dermatitidis exposure in your dog.
Reporting
Blastomycosis in animals is a periodically notifiable in Ontario, meaning laboratories in the province must report cases to the Ontario Ministry of Agriculture, Food and Rural Affairs on an annual basis. Cases that are diagnosed clinically based on the animal’s history, clinical signs, chest radiographs and other testing without submission of samples to a laboratory are not reported. The annual number of cases reported has increased from 45 in 2013, to 149 in 2020, but it is unknown if this is due to increased disease or increased laboratory testing of cases. Mapping of reported cases is primarily reflective of where the affected animals live and were diagnosed, but not necessarily where they were exposed (i.e. travel-related), and is therefore not useful for identifying high-risk areas.
What is the risk?
The risk of disease posed by blastomycosis in dogs to the general population, as well as those typically considered higher risk for infections, is:

Even though transmission of infection from a dog to a person is very unlikely, infection in a dog indicates the fungus is in the environment where the dog has been, and people who were in the same environment could have also been exposed and may be at risk for infection.
Individuals with compromised immune systems (e.g. HIV/AIDS, transplant and cancer patients) are more susceptible to many kinds of infections. Infants and young children (less than 5 years old) may have closer contact with pets (and contaminated soil, through play), which may increase the potential for exposure to the fungus. Young children should be supervised when playing with animals, and an adult should ensure that they wash their hands afterwards. Pets should not be allowed to lick broken skin or any person’s face.
Additional information:
Hunter & Ward. Blastomycosis in dogs. VCA Canada Animal Hospitals. Accessed Jan-2022.
Taboada, 2018. Blastomycosis. Merck Veterinary Manual. Accessed Jan-2022.
Evason & Stull, 2020. Blastomycosis: Information for dog owners (handout). The Ohio State University. Accessed Jan-2022
Other References and image sources:
US Centers for Disease Control. Where blastomycosis comes from. Last reviewed Jan-2021.
Litvinjenko & Lunny, 2017. Blastomycosis hospitalizations in northwestern Ontario: 2006–2015. Can Commun Dis Rep. 43(10):200-5.
CDC Public Health Image Library http://phil.cdc.gov/phil/home.asp

